Insurance is a industry running on a stress fracture: the pressure to deliver a human, compliant experience when policyholders need you most, and the manual grind of chasing claims that should have paid weeks ago. Intelligent Contacts changes the equation by replacing disconnected systems with a single platform for every claim, billing, and communication need.

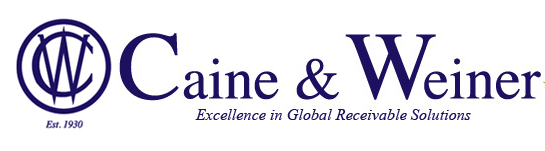





Deploy additional capacity faster in the cloud than provisioning new on-premises servers.
Surface claim history and prior interactions automatically the moment a call connects.
Connect natively to the claims management, billing, and CRM platforms you already run.
Move from fragmented tools to a unified console without the typical implementation delays.
Route follow-up tasks based on payer, denial type, and appeal deadlines automatically.

Route calls based on policy type, history, and intent to reduce unnecessary transfers.
Capture and store every interaction with automated redaction for sensitive health and card info.
Customer frustration during the claims process is a direct driver of churn. We provide answers 24/7 so your team has the full picture before the conversation starts.
Self-Service
Knowledge Gaps
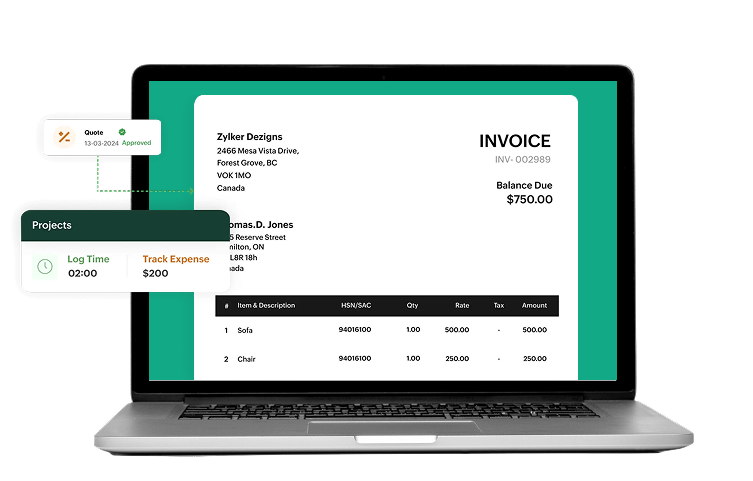
Nearly 20% of all claims are denied, and as many as 60% are never resubmitted. We stop the revenue leak with an outbound engine that prioritizes aged claims before appeal windows close.
Denied Claims
Aged Workflows

Don’t let technical friction get in the way of loyalty. We make it easy for policyholders to resolve balances on their own terms with secure, friction-free payment options.
PCI Compliance
Mobile Payments

Yes. The platform is designed around insurance-specific workflows: inbound claims routing, multi-state compliance, and outbound premium collection.
It replaces spreadsheets with a systematic engine. It tracks every touch and disposition, flagging claims approaching appeal deadlines so nothing falls off the radar.
Precisely. HIPAA, TCPA, and state-specific regulations are enforced at the platform level. When rules change, the platform updates—not your training manual.
For routine questions like status and balance, yes. This frees your team to handle the complex, high-stakes claims where a human touch is non-negotiable.

Equip your team with a high-performance suite built for regulated, high-stakes environments. By unifying your claims, billing, and communication history into a single console, you eliminate duplicate data entry and ensure your team has the full picture before every conversation.
Get Deployed in Days, Not Months.
No capital expense. No complex
installs.
Get Deployed in Days, Not
Months. No capital expense. No
complex installs.

VP of Claims Operations

Director of Revenue Cycle

SVP of Customer Experience
Intelligent Contacts connects easily to your existing tech stack—whether it’s your CRM, EHR, billing system, or custom in-house software. No middleware nightmares. No long waits. Just fast, secure integrations that work.









Protect sensitive health and financial data automatically in every recording.
Enforce opt-in and opt-out rules systematically across voice, text, and email.
Capture every emergency notification and mass alert with timestamped documentation.

By unifying your tools, you eliminate manual friction and empower your team to protect both policyholders and your bottom line. You don’t need more vendors; you need an upgrade your operations team can own today.
Transactions processed
Service Uptime
Faster Resolution and Payment Cycles



Get instant access and explore the platform at your own pace
We use cookies to personalize content, provide features, and analyze our traffic. You can change your preferences at any time. For more information, please see our Privacy Policy and Cookie Policy. Privacy Policy